Augmented Reality (AR) in Surgery: Real-World Applications & Future Scope
Augmented Reality (AR) in Surgery Real-World Applications & Future Scope
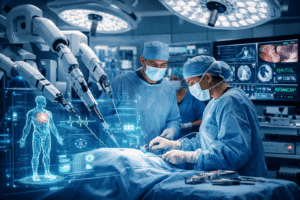
The operating room has long been a place where precision, expertise, and split-second decisions determine patient outcomes. Today, augmented reality is transforming this critical environment by overlaying digital information directly onto the surgeon’s view of the patient, creating an enhanced surgical field that combines the physical and digital worlds. This technology is no longer science fiction—it’s becoming an integral part of modern surgical practice across specialties worldwide.
As we navigate through 2026, augmented reality has evolved from experimental trials to practical clinical applications that are improving surgical accuracy, reducing complications, and enhancing patient education. Leading medical centers worldwide are integrating AR headsets and projection systems into their operating rooms, fundamentally changing how surgeons visualize anatomy, plan procedures, and execute complex operations.
Understanding Augmented Reality in Surgery
Augmented reality overlays digital information—such as three-dimensional medical images, anatomical landmarks, and surgical guidance—onto the real-world view of the surgical field. Unlike virtual reality, which creates completely artificial environments, AR enhances reality by adding layers of digital content while maintaining the surgeon’s connection to the physical patient and operating room.
The key distinction between AR and other technologies is crucial to understand. Virtual reality completely replaces real surroundings with computer-generated environments, while augmented reality incorporates digital imagery within the actual environment. Extended reality serves as an umbrella term describing both technologies and their hybrid applications.
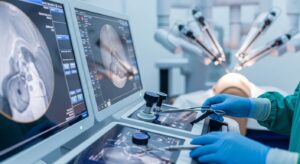
In surgical settings, AR technology typically uses head-mounted displays or projection systems that present three-dimensional computed tomography and MRI scans directly within the surgeon’s field of view. This integration allows surgeons to transition virtual surgical plans seamlessly into the operating room, providing better visualization of the operative field and helping identify structures that would otherwise be difficult to see precisely.
Current AR Technologies in Operating Rooms
Several advanced AR platforms are currently being deployed in surgical environments, each offering unique capabilities and approaches to augmented surgical visualization.
Microsoft HoloLens 2
The Microsoft HoloLens 2 has emerged as a frontrunner in medical AR applications, particularly in neurosurgery, orthopedic surgery, and otolaryngology. This head-mounted device features holographic lenses with 2K resolution per eye and a 52-degree field of view, supporting intuitive interactions through hand tracking, eye tracking, and voice commands.
The HoloLens uses see-through technology with transparent lenses that allow direct viewing of the real environment while superimposing holograms through optical waveguides. This approach ensures high fidelity in perceiving the real world with natural interaction and low latency. Surgeons wearing the device during procedures report satisfaction with image quality, scoring it at 85 out of 100 points on average, and accuracy of virtual objects at 84 out of 100 points.
The device integrates seamlessly with Microsoft’s suite of enterprise tools, including Azure cloud services and Dynamics 365, making it particularly valuable for hospitals already using Microsoft infrastructure. The HoloLens provides 2-3 hours of active use per charge and features a flip-up visor allowing surgeons to quickly switch between AR-enhanced and normal vision.
Apple Vision Pro
Apple’s entry into the medical AR space with the Vision Pro represents a significant technological leap. Introduced in 2023 and priced at $3,499, this mixed reality headset uses pass-through technology with cameras capturing the real environment and projecting it onto screens where virtual elements blend with real-time video feeds.
The Vision Pro offers superior display quality with exceptional pixel density and clarity, advanced eye-tracking capabilities, and precise hand gesture recognition. Its spatial computing capabilities allow physicians to view up to eight screens simultaneously during procedures, streamlining data visualization and reducing the need to look away from the surgical field.
Stanford Medicine physicians are among the first to integrate Vision Pro into surgical practice, using the technology to enhance real-time data visualization during operations. The device’s high-resolution displays and immersive sound quality, combined with seamless integration into Apple’s ecosystem, make it particularly appealing for medical centers already invested in Apple infrastructure.
Recent comparative studies between HoloLens 2 and Apple Vision Pro in orthopedic surgery demonstrate that both devices enable surgeons to access real-time planning during procedures, improving accuracy and reducing operating room time. The choice between platforms often depends on institutional preferences, existing technology infrastructure, and specific surgical requirements.
Projected Augmented Reality Systems
Beyond head-mounted displays, projected augmented reality offers an alternative approach that projects digital surgical information directly onto the operative field. This hands-free, headset-free platform is universally visible to all surgical team members, addressing some limitations of head-mounted systems.
PAR systems use structured light scanners and depth cameras to generate digital 3D surface reconstructions of patient anatomy, then project relevant surgical planning information directly onto the patient’s body. This technology has proven particularly valuable in reconstructive surgery, where projection-based systems display flap templates onto cutaneous defects with superior geometric accuracy compared to freehand surgeon markings.
Real-World Surgical Applications
Augmented reality technology is being applied across virtually every surgical specialty, with particularly impressive results in areas requiring exceptional precision and anatomical visualization.
Neurosurgery: Leading the AR Revolution
Neurosurgery has been at the forefront of surgical AR adoption. The field’s reliance on precise diagnostic imaging and millimeter-level accuracy makes it ideal for AR augmentation. Neurosurgeons use AR to visualize multiple 3D datasets superimposed in perfect harmony over the surgical site, including brain structures, blood vessels, tumors, and planned surgical pathways.
During procedures, AR systems provide virtual navigation as surgeons dissect and examine patient anatomy. The technology helps identify critical structures, suggests optimal approaches based on pre-operative planning, and alerts teams to proximity of vital anatomical features. For complex procedures like deep brain stimulation, where millimeter-to-submillimeter accuracy in electrode placement is crucial, AR guidance represents a significant advancement over traditional navigation methods.
Mixed reality simulations combining AR and VR technologies are increasingly used in neurosurgical education at medical schools, allowing trainees to practice complex procedures repeatedly without patient risk.
Spine Surgery: Enhanced Precision for Delicate Procedures
Spine surgeons benefit immensely from AR’s portability and ability to project images into the real world via portable overhead displays and direct projections. The technology makes pedicle screw placement significantly easier and more accurate during operations. Surgeons using AR during spine procedures do not need to take their eyes off the patient to reference imaging, maintaining focus on the surgical field while still accessing critical anatomical information.
AR systems visualize pre-planned screw routes as holographic overlays during procedures, increasing placement accuracy and reducing the risk of nerve damage or improper positioning. The technology also assists with lumbar pedicle screw replacement and other complex spinal procedures where 3D visualization provides substantial benefits.
Orthopedic Surgery: From Planning to Execution
Orthopedic surgeons use AR for joint replacements, fracture repairs, and complex reconstructive procedures. The technology allows surgeons to engage with patient-specific anatomical structures in three-dimensional environments, improving preoperative planning accuracy and intraoperative decision-making.
For procedures like shoulder arthroplasty, AR headsets display holographic 3D models of the patient’s anatomy that can be moved, rotated, scaled, and positioned using contactless hand gestures and voice commands. This interactive capability helps surgeons understand complex anatomical relationships and plan optimal implant positioning before making any incisions.
Clinical feasibility studies demonstrate that surgeons are generally satisfied with AR technology in orthopedic procedures, finding it particularly valuable for complex cases involving significant anatomical variation or previous surgical alterations.
Otolaryngology and Craniofacial Surgery
Ear, nose, and throat surgeons along with craniofacial specialists have established dedicated extended reality research groups to apply AR overlays to complex surgical procedures. The technology helps surgeons navigate intricate anatomical spaces where traditional visualization is challenging.
Before surgical procedures, patients can experience AR benefits themselves. Using extended reality systems, patients can take virtual trips inside their own anatomy, seeing three-dimensional images of their skulls, identifying where implants will be placed, and understanding what the surgery will accomplish. This application significantly improves patient comprehension and informed consent.
General and Laparoscopic Surgery
In general surgery and laparoscopic procedures, AR technology provides real-time guidance by overlaying critical anatomical information onto the surgical field. Surgeons performing procedures like cholecystectomy or hernia repair benefit from enhanced visualization of blood vessels, bile ducts, and other structures that must be preserved.
Studies examining AR applications in robotic general surgery show promising results, with the technology creating integration of preoperative 3D models into live intraoperative views, providing interactive visual interfaces rather than simple operative fields. This approach enables precision surgery with improved oncological outcomes and reduced complications.
Benefits Transforming Surgical Practice
The integration of augmented reality into surgical practice delivers measurable benefits across multiple dimensions of patient care and surgical efficiency.
Enhanced Surgical Precision and Accuracy
AR technology provides surgeons with millimeter-level precision by overlaying exact anatomical information directly onto their view of the patient. This enhanced visualization allows for more accurate incisions, precise instrument placement, and better preservation of healthy tissue while completely addressing surgical targets.
Computer vision technology integrated into AR systems can detect when surgical sponges or instruments are inadvertently left inside patients, prompting teams to perform final counts before closing incisions. This error prevention capability represents a significant patient safety advancement.
Reduced Operative Time and Complications
Real-time surgical guidance through AR systems reduces the time surgeons spend mentally translating two-dimensional imaging into three-dimensional anatomical understanding. This efficiency translates to shorter operative times, reduced anesthesia exposure for patients, and improved operating room throughput.
Studies demonstrate that procedures performed with AR assistance achieve reductions in both operative time and intraoperative complications compared to traditional approaches. Minimally invasive surgeries facilitated by AR visualization result in smaller incisions, less blood loss, reduced post-operative pain, and significantly shorter hospital stays.
Improved Patient Education and Consent
AR technology revolutionizes how surgeons communicate with patients about upcoming procedures. Instead of explaining complex surgeries using two-dimensional diagrams or verbal descriptions, surgeons can show patients three-dimensional AR visualizations of their own anatomy and the planned surgical approach.
Patients wearing AR headsets can see floating 3D images of their anatomical structures, point to specific areas to see detailed views, and watch simulations of how surgeons will address their conditions. Studies show that AR-enhanced patient education results in better mental comprehension of complex concepts, superior visualization of anatomical structures, and improved understanding of what operations involve.
This enhanced communication leads to more meaningful informed consent, reduced patient anxiety, and more realistic expectations about surgical outcomes and recovery processes.
Training and Skill Development
AR technology has transformed surgical education by allowing trainees to practice on digital replicas of organs and anatomical structures. Medical students and residents can repeat procedures until achieving mastery while instructors monitor progress through AR dashboards. Mistakes in virtual simulations carry no real consequences, creating safe learning environments.
Remote guidance and tele-mentoring using AR has been successfully applied to various surgical specialties, accelerated by pandemic-era restrictions on in-person training. AR-based remote surgical education allows expert surgeons to guide trainees through complex procedures regardless of geographic separation, democratizing access to specialized surgical training.
The ability to save and review procedures completed on AR platforms enables pre-operative learning where learners preview exactly how specific cases are conducted, amplifying learning opportunities and efficiency during hands-on surgery.
Challenges and Limitations
Despite impressive progress, several challenges must be addressed before AR technology achieves widespread surgical adoption.
Technical and Hardware Limitations
Current AR devices face constraints in field of view, display resolution, and brightness that impact visual fidelity. Some optical see-through displays struggle with depth perception and occlusion between virtual and real content. While video see-through systems like Apple Vision Pro provide more possibilities for seamlessly integrating virtual elements, they introduce potential latency issues that could be problematic during rapidly evolving surgical situations.
Achieving millimeter-to-submillimeter clinical accuracy remains challenging, particularly for applications like neuronavigation where positioning errors could have serious consequences. Some studies examining AR systems for screw placement in orthopedic surgery conclude that accuracy improvements are still needed for routine clinical use.
The inability to wear AR headsets simultaneously with loupe magnification represents a significant barrier, as many surgeons rely on magnification for enhanced visualization during procedures. Additionally, exclusive visualization to the headset wearer limits the collaborative nature of surgery, though projected AR systems address this limitation.
Ergonomic and Comfort Concerns
Wearing AR headsets for extended periods can cause physical discomfort, particularly during lengthy procedures. Weight distribution, pressure points, and heat generation from active cooling systems all contribute to user fatigue. Some surgeons report that prolonged headset use leads to neck strain, headaches, or general discomfort that could impact concentration during critical surgical moments.
The closed console design of some AR systems can create feelings of isolation or claustrophobia, while open designs may not provide sufficient immersion for some applications. Finding the optimal balance between comfort, functionality, and surgical effectiveness remains an ongoing challenge.
Sterilization and Operating Room Integration
Integrating AR devices into sterile operating room environments presents practical challenges. Sterilization requirements are stringent, yet some manufacturers recommend against using isopropyl alcohol or other standard solvents for cleaning their devices. This constraint requires developing specialized cleaning protocols or protective barriers that maintain sterility without damaging sensitive electronics.
Active cooling systems in devices like Apple Vision Pro and Magic Leap potentially compromise sterile airflow patterns in operating rooms, raising concerns about infection risk. While some AR devices have received certification for operating room use, achieving appropriate regulatory approval and medical device classification for all AR systems remains an ongoing process.
Cost and Accessibility
AR headsets represent significant capital investments, with devices like HoloLens 2 and Apple Vision Pro priced between $3,500 and $4,950. These costs, combined with necessary software development, staff training, and ongoing support expenses, place AR technology beyond reach for many smaller hospitals and healthcare facilities in resource-limited settings.
This economic barrier creates disparities in access to AR-enhanced surgical care, potentially widening gaps between well-resourced academic medical centers and community hospitals serving underserved populations.
Training Requirements and Learning Curves
Surgical teams require comprehensive training to effectively use AR systems. Learning to interact with holographic interfaces, interpret overlaid information, and integrate AR into surgical workflows demands time and dedicated instruction. During the learning period, procedures may take longer and the technology’s benefits may not be fully realized.
Resistance to change among experienced surgeons accustomed to traditional approaches represents another adoption challenge. Demonstrating clear value and building confidence in the technology through gradual implementation and positive early experiences is essential for successful institutional adoption.
The Future of Augmented Reality in Surgery
Looking beyond current applications, several emerging trends promise to further transform surgical practice through augmented reality.
Artificial Intelligence Integration
The convergence of AR and artificial intelligence will create unprecedented surgical support systems. AI algorithms will analyze real-time video feeds from AR cameras, automatically identifying anatomical structures, predicting optimal surgical approaches, and alerting surgeons to potential complications before they become apparent through traditional observation.
Machine learning models trained on thousands of surgical procedures will provide context-aware guidance tailored to individual patient anatomy and specific procedural scenarios. This intelligent assistance will help democratize surgical expertise, enabling less experienced surgeons to perform complex procedures safely while giving experts tools to push boundaries.
5G and Remote Surgical Collaboration
High-speed, low-latency 5G networks combined with AR technology will enable true international surgical collaboration. Expert surgeons located anywhere in the world will virtually participate in complex procedures, providing real-time guidance through shared AR interfaces visible to the operating team.
This capability will be particularly valuable for rare or highly specialized procedures where expertise is concentrated in a few global centers. Surgeons in resource-limited settings will gain access to world-class guidance, while experts will expand their impact beyond their physical locations.
Haptic Feedback Integration
Future AR systems will incorporate advanced haptic feedback, allowing surgeons to feel virtual anatomical structures and receive tactile guidance during procedures. This sensory integration will combine visual AR overlays with physical sensations, creating more complete and intuitive surgical interfaces.
Haptic technology will help surgeons understand tissue density, optimal suture tension, and safe manipulation forces, further reducing the risk of tissue damage and improving surgical outcomes.
Wireless and Lighter Form Factors
Next-generation AR devices will be significantly lighter and completely wireless, addressing current ergonomic limitations. Battery technology improvements will extend active use time, while advances in display technology will increase resolution and field of view without adding weight or bulk.
These improvements will make AR systems comfortable for even the longest surgical procedures while maintaining or improving visual quality and functionality.
Standardization and Interoperability
As AR technology matures, industry standards for medical AR applications will emerge, ensuring different platforms can share data and work with common surgical planning software. This interoperability will reduce vendor lock-in, lower costs through competition, and accelerate innovation by allowing developers to create applications compatible with multiple AR devices.
Regulatory frameworks will evolve to address AR-specific considerations while ensuring patient safety and effective oversight of this rapidly advancing technology.
FAQS
How does augmented reality differ from virtual reality in surgical applications?
AR overlays digital information onto the real surgical field, allowing surgeons to see both the patient and computer-generated guidance simultaneously. VR creates completely artificial environments, typically used for surgical training and planning rather than actual procedures.
What are the main AR devices currently used in operating rooms?
Microsoft HoloLens 2 and Apple Vision Pro are the primary head-mounted AR devices used in surgical settings, along with projected AR systems that display information directly onto the operative field. Each platform offers different strengths in resolution, field of view, and integration capabilities.
Is AR surgery safer than traditional approaches?
Studies demonstrate that AR-assisted surgery can improve precision, reduce complications, and shorten operative times compared to traditional methods. However, safety depends on proper training, appropriate patient selection, and choosing procedures where AR provides clear benefits over standard techniques.
How much does AR surgical technology cost?
AR headsets range from approximately $3,500 to $4,950, with additional costs for specialized medical software, training, and ongoing support. Total implementation costs vary significantly based on institutional size, planned applications, and integration with existing systems.
Will AR technology replace traditional surgical skills?
AR augments rather than replaces surgical expertise. The technology provides enhanced visualization and guidance, but skilled surgeons remain essential for decision-making, adapting to unexpected situations, and executing precise surgical techniques. AR is a tool that amplifies human capability rather than substituting for it.
Conclusion
Augmented reality is transforming surgery from an art based primarily on human perception and skill into a precision science enhanced by digital intelligence. The technology overlays critical anatomical information directly onto surgeons’ views of patients, improving visualization, reducing errors, and enabling procedures that would be extremely challenging or impossible using traditional approaches.
Current AR platforms like Microsoft HoloLens 2 and Apple Vision Pro are being successfully deployed across surgical specialties including neurosurgery, spine surgery, orthopedics, otolaryngology, and general surgery. These systems demonstrate measurable benefits in surgical precision, operative efficiency, patient education, and surgical training.
Challenges remain—technical limitations in accuracy and display quality, ergonomic concerns during prolonged use, sterilization requirements, high costs, and training needs all present barriers to universal adoption. However, the trajectory is clear: AR technology is improving rapidly while costs decrease and user experience enhances.
The future promises even more dramatic advances as artificial intelligence integration creates intelligent surgical guidance, 5G networks enable global collaboration, haptic feedback provides tactile sensations, and lighter wireless devices improve comfort. Standardization and interoperability will accelerate adoption while regulatory frameworks ensure safety.
For patients, AR-enhanced surgery means safer procedures, better outcomes, and improved understanding of their care. For surgeons, it provides powerful tools that amplify expertise and enable continuous learning. For healthcare systems, AR represents an investment in the future of surgical excellence.
As we progress through 2026 and beyond, augmented reality will transition from innovative technology to standard expectation in surgical care, fundamentally changing how operations are planned, performed, and perfected worldwide.
Disclaimer:
”The information provided on this website is for general informational and educational purposes only. All content is published in good faith and is intended to offer helpful guidance to readers worldwide. However, we make no guarantees about the completeness, reliability, or accuracy of the information presented.”