Next-Generation Surgical Technologies Shaping the Future of Operating Rooms
Advanced surgical technologies shaping the future of modern operating rooms
The modern operating room is undergoing a profound transformation driven by rapid advancements in surgical technology. What was once a space dominated by manual instruments and conventional imaging has evolved into a highly integrated, data-driven environment. Next-generation surgical technologies are redefining how procedures are planned, performed, and evaluated, with the primary goals of improving precision, enhancing patient safety, and optimizing clinical outcomes.
These advancements are closely connected with the growing role of artificial intelligence in surgery, which is enabling surgeons to make data-driven decisions, improve accuracy, and enhance patient safety throughout the surgical workflow.
For surgeons, physicians, and medical students, understanding these emerging technologies is essential. The operating room of the future is not defined by a single innovation but by the seamless integration of artificial intelligence, robotics, advanced imaging, smart systems, and digital infrastructure.
The Evolution of the Modern Operating Room
Traditional operating rooms relied heavily on the surgeon’s experience, visual judgment, and manual dexterity. While these elements remain central, modern surgical practice increasingly depends on technology to support complex decision-making. The shift toward minimally invasive techniques, value-based healthcare, and patient-centered outcomes has accelerated the adoption of next-generation surgical systems.
Today’s operating rooms are evolving into intelligent surgical ecosystems where real-time data, automation, and advanced visualization work together to support surgical teams.
Artificial Intelligence as a Core Surgical Technology
Artificial intelligence has become a foundational component of next-generation operating rooms. AI systems analyze large volumes of clinical data, including medical imaging, electronic health records, and intraoperative video feeds, to support surgical decision-making.
In preoperative settings, AI enhances diagnostic accuracy and surgical planning by identifying anatomical variations and predicting procedural complexity. During surgery, AI-powered computer vision systems assist with anatomical recognition and procedural monitoring. Postoperatively, predictive analytics help identify early signs of complications and guide recovery planning.
Rather than replacing surgeons, artificial intelligence functions as a clinical decision-support tool, augmenting human expertise and reducing variability in surgical care.
Robotic-Assisted Surgery and Precision Enhancement
Robotic-assisted surgery represents one of the most visible advancements shaping the future of operating rooms. Modern robotic platforms provide enhanced dexterity, tremor filtration, and improved visualization, particularly in minimally invasive procedures.
Next-generation robotic systems are increasingly integrated with AI algorithms that optimize instrument movement, suggest procedural pathways, and improve surgical consistency. Many of these innovations are built upon the evolution of robotic-assisted surgical systems, which continue to redefine minimally invasive procedures through enhanced precision, stability, and improved visualization. These systems enable surgeons to perform complex procedures with greater accuracy while minimizing tissue trauma.
As robotic platforms continue to evolve, they are becoming more adaptable, compact, and interoperable, making them a central element of future surgical environments.
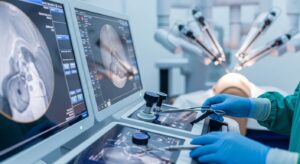
Advanced Imaging and Visualization Technologies
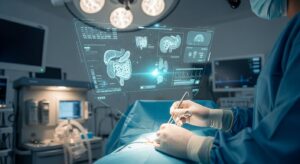
High-quality visualization is critical to surgical success, and next-generation operating rooms are leveraging advanced imaging technologies to improve intraoperative clarity. Innovations such as real-time 3D imaging, augmented reality overlays, and fluorescence-guided surgery allow surgeons to visualize anatomical structures with unprecedented detail.
Augmented reality systems can project digital anatomical data directly into the surgical field, enhancing spatial awareness without disrupting workflow. These technologies are particularly valuable in complex procedures involving delicate structures or limited visual access.
Improved imaging contributes not only to surgical precision but also to reduced operative times and better patient outcomes.
Smart Operating Rooms and Digital Integration
The concept of the smart operating room is central to the future of surgical care. Smart ORs integrate surgical devices, imaging systems, patient monitoring tools, and hospital information systems into a unified digital platform.
This integration enables real-time data sharing, automated documentation, and workflow optimization. Surgeons and clinical teams can access critical patient information instantly, improving coordination and decision-making during procedures.
The concept of smart operating rooms is gaining momentum as hospitals integrate surgical devices, imaging platforms, and patient monitoring systems into unified digital environments. Smart operating rooms also support data collection for quality improvement, research, and surgical education, creating a continuous feedback loop for clinical excellence.
Internet of Medical Things (IoMT) in Surgery
The Internet of Medical Things is expanding the capabilities of operating rooms by connecting surgical instruments, monitoring devices, and support systems. IoMT-enabled devices continuously transmit data related to patient vitals, equipment performance, and environmental conditions.
This connectivity enhances patient safety by enabling early detection of abnormalities and equipment issues. It also supports predictive maintenance of surgical devices, reducing downtime and improving operational efficiency.
IoMT plays a crucial role in building resilient, responsive operating room environments.
Digital Twins and Surgical Simulation
Digital twin technology is emerging as a powerful tool in next-generation surgical planning and training. A digital twin is a virtual representation of a patient’s anatomy created using imaging data and physiological information.
Surgeons can use digital twins to simulate procedures, evaluate different surgical strategies, and anticipate potential complications before entering the operating room. This approach supports personalized surgical care and reduces uncertainty in complex cases.
In education, digital twins and advanced simulators provide immersive training environments that improve skill acquisition and procedural confidence.
Data-Driven Surgical Decision-Making
Next-generation operating rooms are increasingly data-centric. Advanced analytics platforms aggregate intraoperative data, procedural metrics, and patient outcomes to support evidence-based decision-making.
These systems help identify best practices, reduce variability in care, and support continuous quality improvement. For surgeons and healthcare institutions, data-driven insights contribute to safer procedures, improved efficiency, and better long-term outcomes.
Cybersecurity and Data Protection in the Operating Room
As operating rooms become more connected, cybersecurity has become a critical consideration. Protecting patient data and ensuring system integrity are essential for maintaining trust and safety.
Next-generation surgical environments incorporate advanced cybersecurity measures, including encrypted data transmission, access controls, and continuous system monitoring. These safeguards are vital for preventing disruptions and protecting sensitive medical information.
Challenges in Adopting Next-Generation Surgical Technologies
Despite their benefits, advanced surgical technologies present several challenges. High implementation costs, infrastructure requirements, and the need for specialized training can slow adoption. Additionally, integrating new technologies into established workflows requires careful planning to avoid disruption.
Ethical considerations, regulatory compliance, and data governance also play a significant role in determining how and when these technologies are deployed. Successful implementation depends on balancing innovation with patient safety and clinical responsibility.
The Future Vision of Operating Rooms
The operating rooms of the future will be intelligent, adaptive, and highly collaborative environments. Surgeons will work alongside AI-driven systems, robotic platforms, and advanced visualization tools that enhance decision-making without replacing human judgment.
Future ORs will emphasize personalization, precision, and efficiency while maintaining the human-centered values of surgical care. As technology continues to evolve, operating rooms will become safer, more predictable, and better equipped to handle complex procedures.
Why Human Expertise Remains Central
While next-generation technologies significantly enhance surgical capabilities, they cannot replace the clinical intuition, ethical reasoning, and empathy of human surgeons. Surgery is as much an art as it is a science, requiring judgment that extends beyond algorithms.
The most successful surgical environments will be those that integrate advanced technology while preserving human leadership and accountability.
Conclusion
Next-generation surgical technologies are reshaping the future of operating rooms by enabling greater precision, improved safety, and data-driven clinical decisions. Artificial intelligence, robotic-assisted systems, advanced imaging, smart OR integration, and digital simulation are collectively transforming surgical practice.
For surgeons, doctors, and medical students, staying informed about these innovations is essential for adapting to the future of surgical care. When implemented responsibly, these technologies have the potential to elevate surgical outcomes while reinforcing the critical role of human expertise.
FAQs
What defines a next-generation operating room?
A next-generation operating room integrates AI, robotics, advanced imaging, and digital systems to enhance surgical precision, safety, and workflow efficiency.
How do smart operating rooms improve surgical outcomes?
Smart ORs provide real-time data integration, improved coordination, and automated workflows that reduce errors and support informed decision-making.
Are robotic surgical systems safe for complex procedures?
Yes. When used by trained surgeons, robotic systems enhance precision and consistency, particularly in minimally invasive and complex surgeries.
What role does AI play in future surgical practice?
AI supports surgical planning, intraoperative guidance, complication prediction, and postoperative care while assisting—not replacing—surgeons.
Will future operating rooms rely entirely on automation?
No. Automation will support surgical teams, but human judgment, skill, and accountability will remain central to surgical care.