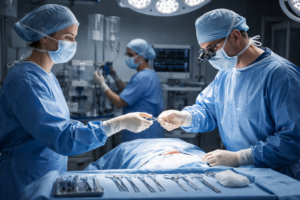
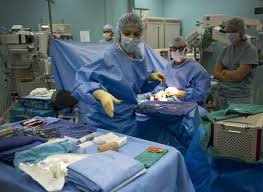
What Minimally Invasive Surgery Actually Is (Explained Simply)
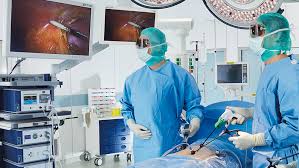
What Minimally Invasive Surgery Actually Is (Explained Simply)
Surgery has long been associated with long recovery times, large scars, and significant pain. But in recent decades, a revolutionary approach called minimally invasive surgery (MIS) has transformed the surgical landscape. In this article, we’ll break down what minimally invasive surgery actually is, how it works, its benefits, and why it’s becoming the preferred choice for many medical procedures around the world.
Understanding Minimally Invasive Surgery
Minimally invasive surgery is a technique where doctors operate through tiny incisions instead of the large cuts typical of traditional surgery. The idea is simple: do more with less trauma to the body. Instead of fully opening a body cavity, surgeons use specialized instruments and cameras to perform complex procedures without causing unnecessary damage to surrounding tissues.
Some of the most common minimally invasive techniques include:
- Laparoscopy – Used for abdominal procedures like gallbladder removal.
- Endoscopy – For internal examinations and certain surgeries.
- Arthroscopy – Commonly used for joint surgeries like knees and shoulders.
- Robotic-assisted surgery – Offers precision beyond human capability.
The ultimate goal of MIS is to make surgery safer, faster, and more comfortable for patients.
How Minimally Invasive Surgery Works
At the core of minimally invasive surgery is precision technology. Surgeons use tools like:
- Endoscopes and laparoscopes – Thin, flexible tubes with cameras that transmit images to a screen.
- Specialized surgical instruments – Designed to operate through tiny incisions.
- Robotic systems – Controlled by the surgeon to perform delicate maneuvers with extreme accuracy.
During the procedure, instead of opening a large area, the surgeon makes small cuts, often less than an inch, and inserts these instruments. The high-definition cameras allow surgeons to see a magnified view of the internal organs, making it easier to navigate complex anatomy.
This technology reduces the need for extensive surgical exposure, lowering the risk of infection, blood loss, and post-operative complications.
Types of Minimally Invasive Surgery
Minimally invasive surgery isn’t a single procedure but a category of techniques. Here are some popular types:
Laparoscopic Surgery
Used for abdominal procedures such as:
- Gallbladder removal
- Hernia repair
- Appendectomy
Surgeons insert a laparoscope through small incisions and operate with tiny instruments. Recovery is typically faster than traditional open surgery.
Endoscopic Surgery
Involves inserting an endoscope through natural openings or small cuts to:
- Remove polyps
- Treat gastrointestinal issues
- Perform ENT procedures
This method avoids major incisions, reducing pain and scarring.
Robotic Surgery
A surgeon controls robotic arms via a console. The robot provides:
- Greater precision
- Tremor filtration
- Better access to hard-to-reach areas
Robotic surgery is common in prostate, cardiac, and gynecological procedures.
Arthroscopic Surgery
Used for joint issues, especially knees, shoulders, and hips. Surgeons insert a camera to:
- Repair torn ligaments
- Remove damaged cartilage
- Improve joint function
Recovery is usually faster, allowing patients to regain mobility sooner.
Benefits of Minimally Invasive Surgery
The rise of MIS is not just a trend—it’s because of real, tangible benefits of Minimally Invasive Surgery. Some major advantages include:
- Smaller scars – Tiny incisions heal faster and leave minimal visible marks.
- Less pain – Patients experience significantly reduced post-operative pain.
- Faster recovery – Many patients return to normal activities in days or weeks.
- Lower infection risk – Reduced exposure of internal tissues decreases complications.
- Shorter hospital stays – Often outpatient or one-night hospital admissions.
- Better cosmetic results – Especially important in procedures affecting appearance.
These benefits make MIS attractive for patients and surgeons alike, improving both safety and patient satisfaction.
Risks and Considerations
No surgery is without risks. While MIS is safer than traditional surgery in many cases, it can still have complications such as:
- Bleeding
- Infection
- Damage to nearby organs
- Anesthesia risks
Additionally, not every patient is a candidate. Some complex conditions may require open surgery to ensure safety. Doctors typically evaluate:
- Patient’s age and overall health
- Specific medical condition
- Previous surgeries and scar tissue
Common Conditions Treated with Minimally Invasive Surgery
Minimally invasive surgery is versatile. Here’s a list of conditions commonly treated:
- Gallstones – Laparoscopic cholecystectomy is standard.
- Appendicitis – Laparoscopic appendectomy reduces recovery time.
- Hernias – Laparoscopic hernia repair minimizes tissue damage.
- Joint injuries – Arthroscopy for knees, shoulders, hips.
- Cancer treatments – Certain tumors can be removed minimally invasively.
- Heart procedures – Some valve repairs and bypass surgeries use MIS techniques.
This wide range demonstrates that MIS is not limited to one area of medicine—it’s a global solution for modern surgical care.
Minimally Invasive Surgery vs. Traditional Surgery
Here’s a comparison to understand why MIS is gaining popularity:
| Feature | Minimally Invasive Surgery | Traditional Surgery |
|---|---|---|
| Incision size | Small (≤1 inch) | Large (several inches) |
| Recovery | Days to weeks | Weeks to months |
| Pain | Mild | Moderate to severe |
| Infection risk | Low | Higher |
| Hospital stay | Short | Longer |
| Scarring | Minimal | Significant |
Clearly, MIS offers faster, safer, and less painful recovery, making it preferable for eligible patients worldwide.
Preparing for Minimally Invasive Surgery
Preparation is key for any surgery, including MIS. Doctors often advise:
- Medical evaluation – Blood tests, imaging, and physical exams.
- Medications review – Some medicines may need to be paused.
- Fasting – Usually required 6–12 hours before surgery.
- Lifestyle adjustments – Stopping smoking or alcohol for better healing.
Proper preparation ensures better outcomes, fewer complications, and a smoother recovery.
Recovery and Aftercare
Recovery from MIS is often quicker than traditional surgery, but it still requires attention:
- Pain management – Over-the-counter or prescribed medication may be needed.
- Wound care – Keep small incisions clean and dry.
- Physical activity – Gradually increase activity as advised by your doctor.
- Follow-up visits – Essential to monitor healing and prevent complications.
Most patients can return to work and daily activities within 1–3 weeks, depending on the procedure.
Technological Innovations in Minimally Invasive Surgery
The field of MIS continues to evolve. New technologies include:
- 3D imaging and virtual reality – Enhances precision and planning.
- Artificial intelligence (AI) – Assists in decision-making and predicting outcomes.
- Single-incision surgery – Minimizes scars further, sometimes leaving nearly invisible marks.
- Robotic advancements – Greater dexterity, precision, and safer procedures.
These innovations make MIS safer, more efficient, and globally accessible, even in countries with advanced healthcare infrastructure.
Global Trends in Minimally Invasive Surgery
MIS is no longer limited to high-income countries. Globally:
- North America and Europe – Widely adopted in hospitals for most surgical specialties.
- Asia – Rapid growth in urban centers; robotic surgery gaining momentum.
- Middle East – Private hospitals lead MIS adoption; government hospitals are catching up.
- Africa and Latin America – Gradual expansion; technology and training are key challenges.
As healthcare improves worldwide, MIS is becoming the gold standard, offering patients shorter recovery, safer outcomes, and less pain.
Costs and Insurance Coverage
While MIS can sometimes be more expensive upfront due to technology and specialized training, it often saves money long-term because:
- Shorter hospital stays
- Reduced need for post-surgery care
- Faster return to work
Insurance coverage for MIS varies by country and procedure. Many global insurers now recognize its benefits and fully or partially cover these surgeries.
Patient Testimonials and Experiences
Patients worldwide report positive experiences with MIS:
- Minimal pain and discomfort
- Quick return to daily life
- Better cosmetic outcomes
- Confidence in undergoing necessary procedures
Such testimonials contribute to growing public awareness and preference for MIS, reinforcing its role as a patient-centered approach.
Future of Minimally Invasive Surgery
The future is bright:
- AI-assisted surgery will make procedures faster and safer.
- Tele-surgery may allow remote operations across countries.
- Nanotechnology could enable surgeries at cellular levels.
As technology advances, MIS will continue to redefine surgical care globally, offering precision, safety, and comfort like never before.
Conclusion
Minimally invasive surgery is a game-changer in modern medicine. By reducing trauma, speeding recovery, and improving patient comfort, it has transformed the way surgery is approached worldwide. Whether through laparoscopy, robotic assistance, or endoscopy, MIS offers a smarter, safer, and more patient-friendly surgical experience.
For anyone facing surgery, understanding MIS can empower you to make informed decisions, discuss options with your doctor, and experience a smoother recovery with minimal complications.
(FAQs)
1. Is minimally invasive surgery painful?
Pain is generally much lower than traditional surgery due to smaller incisions, and most patients manage it with mild medications.
2. Can everyone undergo minimally invasive surgery?
Not everyone. Patients with complex conditions, severe scar tissue, or certain health issues may require traditional surgery.
3. How long does recovery take?
Recovery varies but is usually 1–3 weeks for most procedures, much faster than open surgery.
4. Is MIS more expensive?
It can be slightly higher upfront due to technology but often saves money through shorter hospital stays and faster return to work.
5. Are there long-term benefits of MIS?
Yes. Smaller scars, less risk of infection, and faster recovery contribute to long-term satisfaction and better overall outcomes.
Disclaimer
”The content in this article is for informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of a qualified healthcare provider with any questions regarding a medical condition or surgery.”