How Artificial Intelligence Is Transforming Modern Surgery
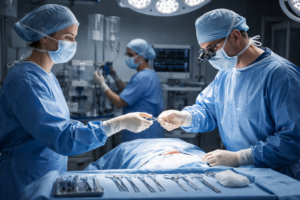
AI-powered technologies enhancing precision and safety in modern surgical procedures
Artificial Intelligence (AI) has rapidly transitioned from an experimental concept to a practical and indispensable tool in modern surgical practice. Today, AI-driven technologies are influencing nearly every stage of the surgical journey—from preoperative evaluation and intraoperative decision-making to postoperative monitoring and surgical education. For surgeons, physicians, and medical students, understanding the role of AI in surgery is now essential for delivering safe, efficient, and evidence-based care.
This article explores how artificial intelligence is transforming modern surgery, highlighting its clinical applications, benefits, limitations, and future direction.
Artificial Intelligence in the Surgical Context
In surgery, artificial intelligence refers to the application of machine learning algorithms, deep learning models, computer vision, and predictive analytics to analyze clinical data and assist surgical teams. These systems process vast amounts of information derived from medical imaging, electronic health records, operative videos, and patient monitoring systems.
Unlike traditional software, AI systems continuously learn from data, allowing them to improve accuracy and adapt to complex clinical scenarios. As a result, AI serves as a clinical decision-support tool rather than an autonomous decision-maker.
Preoperative Applications of AI in Surgery
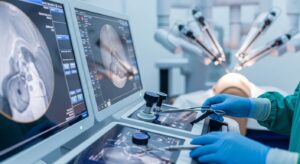
One of the most significant contributions of AI is in preoperative planning. Advanced AI-powered imaging tools analyze radiological data such as CT scans, MRI images, and ultrasounds with a level of precision that supports early diagnosis and accurate surgical mapping. These systems can identify subtle anatomical variations, detect early-stage pathology, and assist surgeons in selecting the most appropriate surgical approach.
AI-based predictive models also play a critical role in assessing surgical risk. By evaluating patient-specific factors—including comorbidities, laboratory values, and prior surgical history—AI can estimate the likelihood of complications, expected recovery duration, and potential postoperative outcomes. This allows for better patient selection, personalized treatment planning, and more informed consent discussions.
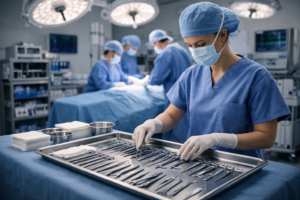
Intraoperative Role of Artificial Intelligence
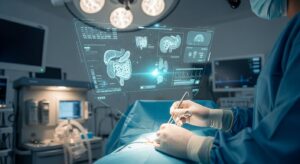
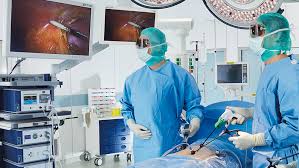
During surgery, AI enhances precision and situational awareness within the operating room. Computer vision technology enables real-time analysis of surgical video feeds, allowing AI systems to recognize anatomical structures, track surgical instruments, and monitor procedural progress. These capabilities help reduce human error and improve consistency in complex procedures.
AI-integrated robotic surgery platforms further extend surgical capabilities. These systems refine hand movements, minimize tremors, and enable greater dexterity during minimally invasive procedures. Importantly, AI does not replace the surgeon but functions as an intelligent assistant that enhances technical performance while preserving full human control.
In certain settings, AI-driven intraoperative guidance systems can provide real-time alerts related to critical anatomical landmarks or abnormal physiological changes. Such feedback supports safer surgical execution and improved patient outcomes.
Postoperative Care and Recovery Optimization
Artificial intelligence continues to add value beyond the operating room. Postoperatively, AI systems analyze patient data in real time to detect early signs of complications such as infection, bleeding, or thromboembolic events. Continuous monitoring enables clinicians to intervene earlier, reducing morbidity and length of hospital stay.
AI also supports personalized postoperative recovery pathways. By predicting pain levels, mobility milestones, and rehabilitation needs, AI helps clinicians design tailored recovery plans that improve patient satisfaction and resource utilization.
Impact of AI on Surgical Education and Training
Surgical education has been significantly enhanced by AI-driven simulation technologies. These platforms offer realistic, data-rich environments where medical students and surgical trainees can practice procedures without patient risk. AI-based performance analytics provide objective feedback on technique, efficiency, and decision-making.
Furthermore, AI allows for standardized assessment of surgical skills by analyzing instrument handling, motion patterns, and procedural timing. This reduces subjectivity in training evaluations and promotes competency-based education.
Clinical Benefits of AI in Modern Surgery
The integration of artificial intelligence into surgical practice has led to measurable clinical improvements. AI contributes to higher surgical accuracy, reduced complication rates, improved patient safety, and more efficient use of healthcare resources. By standardizing best practices and supporting evidence-based decision-making, AI enhances both surgical quality and operational efficiency.
Challenges and Ethical Considerations
Despite its advantages, AI adoption in surgery presents important challenges. AI systems rely heavily on high-quality data, and biased or incomplete datasets can negatively affect predictions and outcomes. Ensuring data diversity and transparency is therefore essential.
Ethical and legal considerations also remain central concerns. Questions surrounding accountability, informed consent, and clinical responsibility must be carefully addressed as AI becomes more integrated into surgical workflows. Additionally, successful implementation requires appropriate training, infrastructure investment, and regulatory oversight to ensure patient safety.
Future Directions of Artificial Intelligence in Surgery
The future of AI in surgery is focused on deeper integration rather than autonomy. Emerging innovations include augmented reality-assisted surgery, digital twin modeling for preoperative simulation, and intelligent operating rooms that respond dynamically to surgical conditions.
These advancements aim to support surgeons with real-time insights while maintaining human judgment as the cornerstone of surgical care. AI is expected to become a standard component of surgical practice, much like imaging and minimally invasive tools today.
Why Artificial Intelligence Will Not Replace Surgeons
Although AI is highly advanced, it lacks clinical intuition, ethical reasoning, and emotional intelligence. Surgery involves complex decision-making, patient communication, and moral responsibility—areas where human expertise remains irreplaceable. AI should be viewed as a powerful extension of surgical capability rather than a substitute for the surgeon.
Conclusion
Artificial intelligence is reshaping modern surgery by enhancing precision, improving safety, and supporting data-driven clinical decisions. Its influence spans preoperative planning, intraoperative assistance, postoperative care, and surgical education. When implemented responsibly, AI has the potential to elevate surgical outcomes while preserving the essential human elements of care.
For surgeons, doctors, and medical students, understanding and embracing AI is vital to staying aligned with the future of surgical practice.
FAQs
How is artificial intelligence currently used in surgery?
AI is used in surgical planning, imaging analysis, robotic assistance, intraoperative guidance, complication prediction, and postoperative monitoring.
2. Is AI-assisted surgery safe for patients?
When properly regulated and used as an assistive tool, AI improves patient safety by enhancing accuracy and reducing errors.
Can AI perform surgery independently?
No. Current AI systems support surgeons but do not operate independently. Human surgeons remain fully responsible for all procedures. Which surgical specialties benefit most from AI?
AI is widely used in minimally invasive surgery, orthopedics, neurosurgery, cardiovascular surgery, and general surgery.
Will AI become a standard part of future surgical practice?
Yes. AI is expected to become a routine component of modern surgical workflows due to its clinical and operational benefits.
Disclaimer:
”The information provided on this website is for general informational and educational purposes only. All content is published in good faith and is intended to offer helpful guidance to readers worldwide. However, we make no guarantees about the completeness, reliability, or accuracy of the information presented.”