Classification of Surgical Instruments: A Complete Guide for Modern Healthcare
Introduction to Surgical Instruments Classification
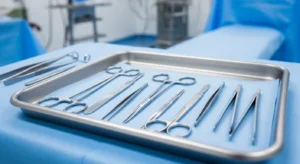
Surgical instruments classification refers to the systematic organization of medical tools based on their function, design, and specific use in surgical procedures. This classification helps healthcare professionals quickly identify and select the right surgical instrument during operations, improving efficiency and accuracy. In modern medicine, where hundreds of instruments are used, proper categorization is essential for smooth workflow in the operating room. It also plays a key role in training medical students by making learning more structured and understandable. Additionally, classification supports sterilization processes and patient safety by ensuring instruments are handled correctly. Overall, it forms the foundation of effective and safe surgical practice worldwide.
What Does Classification Mean in Surgery?
When we talk about classification of surgical instruments, we’re essentially organizing a vast world of medical tools into structured categories based on their function, design, and application. Think of it like organizing a toolbox—except instead of screws and wrenches, we’re dealing with life-saving instruments used in operating rooms across the globe. Without proper classification, even the most experienced surgical team could struggle to find the right tool at the right time.
In surgical practice, classification is not just about naming surgical instruments—it’s about understanding their purpose, behavior, and interaction with human tissue. For example, a scalpel is not just a cutting tool; it is designed for precision, minimal tissue damage, and controlled incisions. Similarly, forceps are not just for holding—they are engineered to handle delicate tissues without causing trauma.
Globally, healthcare systems rely heavily on standardized classification methods to ensure consistency. Whether a surgery is being performed in the United States, Europe, or Asia, the categorization of instruments helps maintain a universal language among medical professionals. This becomes especially important in international collaborations, training programs, and emergency medical situations.
According to the World Health Organization (WHO), structured surgical practices—including proper instrument classification—play a significant role in improving surgical outcomes and reducing complications. This highlights that classification is not just a technical detail; it’s a critical component of patient care.
In simple terms, classification transforms a chaotic collection of tools into an organized system that enhances efficiency, safety, and precision in surgery. It allows surgeons to focus on what truly matters—saving lives—without being slowed down by confusion or inefficiency.
Why Classification is Important in Medical Practice
Now you might be wondering—why put so much emphasis on classification? Can’t surgeons just learn instruments individually? The reality is, modern medicine is far too complex for that approach. With hundreds of instruments available, classification becomes essential for clarity, speed, and accuracy.
One of the biggest advantages is efficiency in the operating room. During surgery, every second counts. A well-classified set of instruments allows surgical teams to quickly identify and access the tools they need. This reduces delays and ensures that procedures run smoothly. Imagine a surgeon asking for a specific clamp and the assistant immediately knowing exactly where it is—that’s the power of proper classification.
Another major factor is training and education. Medical students and surgical trainees rely on classification systems to learn about instruments in a structured way. Instead of memorizing random tools, they understand categories, functions, and relationships. This makes learning faster and more effective.
Classification also plays a key role in infection control and sterilization. Instruments are often grouped based on how they are used and cleaned. For instance, tools that come into contact with sterile body tissues require stricter sterilization protocols. The Centers for Disease Control and Prevention (CDC) emphasizes that proper categorization of medical instruments is crucial for effective sterilization and infection prevention.
From a global perspective, classification supports standardization. Hospitals, manufacturers, and regulatory bodies use classification systems to ensure consistency in design, labeling, and usage. This is particularly important in international healthcare environments where professionals from different backgrounds work together.
In short, classification is not just about organization—it’s about creating a system that improves every aspect of surgical practice, from training to execution to patient safety.
Major Categories of Surgical Instruments
Cutting and Dissecting Instruments
Among all classifications, cutting and dissecting instruments are perhaps the most fundamental. These are the tools that initiate most surgical procedures, making them indispensable in every operating room. Their primary function is to cut through tissues, organs, or other structures with precision and minimal damage.
The most iconic example is the scalpel, a small yet incredibly sharp instrument designed for making clean incisions. Its effectiveness lies in its simplicity and precision. Modern scalpels often feature disposable blades, ensuring maximum sharpness and hygiene for each procedure.
Other important tools in this category include surgical scissors, which are used for cutting tissues, sutures, or dressings. These scissors come in various shapes and sizes, such as straight and curved designs, each suited for specific tasks. Curved scissors, for example, allow better access to deeper areas of the body.
Dissecting instruments also include tools like osteotomes and curettes, which are used for cutting or scraping bone and other hard tissues. These instruments require a high level of control, as they are often used in delicate procedures.
Advancements in technology have introduced laser scalpels and ultrasonic cutting devices, which offer even greater precision and reduced bleeding. These innovations are transforming how surgeries are performed, making procedures less invasive and more efficient.
Globally, these instruments are considered the starting point of any surgical classification system. Their importance cannot be overstated, as they directly impact the success of a procedure. A precise cut can mean faster healing, reduced complications, and better outcomes for patients.
Grasping and Holding Instruments
Once an incision is made, the next step involves handling tissues carefully—and that’s where grasping and holding instruments come into play. These tools are designed to provide stability and control, allowing surgeons to manipulate tissues without causing damage.
The most commonly used instrument in this category is the forceps. These are versatile tools used for gripping, holding, or manipulating tissues and objects. Depending on their design, forceps can be used for delicate tasks, such as handling blood vessels, or for more robust applications.
Another essential instrument is the needle holder, which is used during suturing. It allows surgeons to hold and guide needles with precision, ensuring that stitches are placed accurately. Proper suturing is critical for wound healing and minimizing scarring.
What makes these instruments unique is their ability to balance firmness and gentleness. Too much pressure can damage tissues, while too little can make the procedure difficult. This balance is achieved through careful design and high-quality materials.
Ergonomics also plays a significant role. Modern grasping instruments are designed to reduce hand fatigue, which is especially important during long surgeries. This improves performance and reduces the risk of errors.
From a global perspective, these instruments are indispensable in both basic and advanced surgical procedures. They may not always be in the spotlight, but they are essential for maintaining control and precision throughout the operation.
Clamping and Occluding Instruments
When it comes to controlling bleeding during surgery, clamping and occluding instruments are absolutely critical. Without them, even a minor surgical procedure could quickly turn into a dangerous situation. These instruments are specifically designed to control blood flow, clamp vessels, and temporarily stop circulation in targeted areas, allowing surgeons to work in a clear and controlled field.
The most commonly used instrument in this category is the hemostat. It’s designed to clamp blood vessels and prevent excessive bleeding during surgery. Hemostats come with a locking mechanism, usually a ratchet system, that allows them to stay securely in place without continuous manual pressure. This frees up the surgeon’s hands to focus on other critical tasks.
Another important tool is the vascular clamp, which is used in delicate procedures involving blood vessels. These clamps are engineered with precision to apply just enough pressure to stop blood flow without damaging the vessel walls. This is especially crucial in cardiovascular surgeries, where even slight damage can have serious consequences.
Clamping instruments are also used in procedures involving organs, such as the intestines or lungs, where temporary occlusion is necessary. These tools ensure that surgeons can isolate specific areas and perform procedures safely.
According to guidelines from the U.S. Food and Drug Administration (FDA), surgical instruments used for controlling blood flow must meet strict safety and quality standards to ensure patient safety. This highlights the importance of reliability in this category.
Globally, clamping and occluding instruments are a cornerstone of surgical practice. They not only improve visibility during procedures but also play a vital role in preventing complications. In simple terms, they act as the “control system” of surgery, managing one of the most critical aspects—blood flow.
Retracting and Exposing Instruments
Visibility is everything in surgery. No matter how skilled a surgeon is, they cannot operate effectively without a clear view of the surgical area. That’s where retracting and exposing instruments come into play. These tools are designed to hold back tissues, muscles, or organs, providing better access and visibility to the surgical site.
The most well-known instrument in this category is the retractor. Retractors can be handheld or self-retaining. Handheld retractors require an assistant to hold them in place, while self-retaining retractors are designed to stay in position on their own. This makes them especially useful in long procedures where maintaining a clear view is essential.
Another commonly used instrument is the speculum, which is used to open body cavities for examination and surgery. It is widely used in gynecology and ENT (ear, nose, and throat) procedures.
Retracting instruments must be designed with precision and care. Applying too much pressure can damage tissues, while insufficient retraction can limit visibility. This balance is crucial for successful surgical outcomes.
Modern advancements have introduced retractors with integrated lighting systems, which enhance visibility even further. This is particularly useful in minimally invasive surgeries, where the surgical field is limited.
The Royal College of Surgeons emphasizes the importance of proper exposure during surgical procedures, noting that clear visibility significantly reduces the risk of errors and complications.
Globally, retracting instruments are essential for improving surgical efficiency and accuracy. They may not directly interact with the surgical target, but they create the conditions necessary for success. Think of them as the stage crew that ensures everything is visible and accessible for the main performance.
Functional Classification of Surgical Instruments
Probing and Dilating Instruments
Not all surgical instruments are used for cutting or holding—some are designed to explore and prepare the body for procedures. This is where probing and dilating instruments come into play. These tools are used to examine body cavities, measure depths, or gently expand openings to allow access for other instruments.
Probes are slender, flexible instruments used to explore wounds or body cavities. They help surgeons assess the depth, direction, and condition of a surgical site. For example, a probe can be used to locate a foreign object or determine the extent of a wound.
On the other hand, dilators are used to widen narrow passages in the body, such as blood vessels or ducts. This is often necessary before inserting other instruments or performing certain procedures. Dilators come in various sizes, allowing gradual expansion without causing damage.
These instruments require a high level of precision and care, as they are often used in sensitive areas. Their design ensures minimal discomfort and maximum safety for patients.
According to MedlinePlus, diagnostic and exploratory tools like probes play a crucial role in surgical planning and execution, helping healthcare professionals make informed decisions.
Globally, probing and dilating instruments are used in a wide range of specialties, from general surgery to urology and gynecology. They may not be as widely recognized as scalpels or forceps, but their role is equally important.
In simple terms, these instruments act as the “explorers” of surgery, helping surgeons understand the terrain before taking action.
Suturing and Stapling Instruments
Once a surgical procedure is complete, the focus shifts to closing the wound, and that’s where suturing and stapling instruments come in. These tools are essential for ensuring proper healing and minimizing the risk of infection or complications.
The most common instrument in this category is the needle holder, which is used to guide sutures through tissues. It provides a firm grip on the needle, allowing precise placement of stitches. Suturing is a delicate process that requires skill and accuracy, as it directly impacts how well a wound heals.
In addition to traditional sutures, modern surgery often uses surgical staplers. These devices are designed to close wounds quickly and efficiently, especially in procedures involving large areas. Staplers are commonly used in gastrointestinal and thoracic surgeries.
One of the advantages of stapling is speed. It allows surgeons to close wounds faster, reducing operating time and minimizing the risk of infection. However, sutures are still preferred in many cases where precision is required.
The Mayo Clinic highlights that proper wound closure techniques are essential for reducing complications and promoting faster recovery.
Globally, these instruments are a vital part of every surgical procedure. They represent the final step in surgery, ensuring that the patient’s body can begin the healing process effectively.
Classification Based on Surgical Specialties
General Surgery Instruments
General surgery instruments are the backbone of most surgical procedures. These tools are versatile and can be used across a wide range of operations, from minor procedures to more complex surgeries. They include basic instruments like scalpels, forceps, scissors, and retractors.
What makes general surgery instruments unique is their adaptability. They are not designed for a single specific procedure but can be used in various contexts. This makes them essential in hospitals and clinics worldwide.
These instruments are often the first ones that medical students learn about, as they form the foundation of surgical practice. Understanding their functions and classifications is crucial for anyone entering the medical field.
Globally, general surgery instruments are standardized to ensure consistency and reliability. This allows healthcare professionals to work efficiently, regardless of their location.
Specialized Surgical Instruments
In contrast to general instruments, specialized surgical instruments are designed for specific medical fields. These include tools used in cardiology, neurology, orthopedics, and more.
For example, neurosurgery requires extremely delicate instruments for working on the brain and spinal cord, while orthopedic surgery uses heavy-duty tools for cutting and shaping bones.
The Johns Hopkins Medicine resource emphasizes that specialized instruments are essential for handling the unique challenges of different medical disciplines.
These instruments highlight the diversity and complexity of modern medicine. They are tailored to meet specific needs, ensuring that each procedure is performed with the highest level of precision.
Classification Based on Usage and Design
Reusable vs Disposable Instruments
One of the most practical ways to classify surgical instruments is based on their usage—whether they are reusable or disposable. This distinction might seem simple at first glance, but it has a major impact on cost, safety, sustainability, and global healthcare accessibility.
Reusable surgical instruments are designed to be used multiple times after proper cleaning and sterilization. These are typically made from durable materials like high-grade stainless steel or titanium, allowing them to withstand repeated sterilization cycles without losing their functionality. Instruments such as forceps, scissors, and clamps are commonly reusable and are widely used in hospitals around the world.
The biggest advantage of reusable instruments is cost-effectiveness over time. Although the initial investment may be higher, their long lifespan makes them more economical in the long run. This is especially important in developing countries, where healthcare budgets are often limited. However, the downside is that they require strict sterilization protocols. If not cleaned properly, they can become a source of infection.
On the other hand, disposable (single-use) instruments are designed to be used once and then discarded. These are often made from plastic or lower-cost metals and come pre-sterilized. Examples include disposable scalpels, syringes, and certain types of forceps.
The key advantage here is infection control. Since these instruments are used only once, the risk of cross-contamination is significantly reduced. This makes them particularly useful in high-risk environments or emergency situations. According to the Centers for Disease Control and Prevention (CDC), single-use instruments can play a crucial role in reducing healthcare-associated infections when used appropriately.
However, disposable instruments also come with challenges, particularly in terms of environmental impact. The increasing use of single-use medical tools has raised concerns about medical waste and sustainability. Many healthcare systems are now exploring eco-friendly alternatives to address this issue.
Globally, both types of instruments are used depending on the healthcare setting, resources, and specific needs. In high-income countries, there is often a balance between reusable and disposable tools, while in resource-limited settings, reusable instruments are more common due to cost constraints.
In simple terms, this classification highlights a key trade-off between cost, safety, and sustainability, making it one of the most practical considerations in modern surgical practice.
Ergonomic and Smart Instruments
As technology continues to evolve, surgical instruments are no longer just static tools—they are becoming smarter, more efficient, and user-friendly. This has led to a new classification based on design innovation, including ergonomic and smart surgical instruments.
Ergonomic instruments are designed with the user in mind—specifically, the surgeon. These tools aim to reduce hand fatigue, improve grip, and enhance precision during long procedures. For example, many modern instruments feature non-slip handles, lightweight materials, and optimized shapes that fit comfortably in the hand.
Why does this matter? Because surgeries can last for several hours, and even slight discomfort can affect a surgeon’s performance. Ergonomic designs help maintain consistency and accuracy, which ultimately benefits the patient.
Then we have smart surgical instruments, which represent the cutting edge of medical innovation. These tools are equipped with sensors, connectivity features, and sometimes even AI integration. They can provide real-time feedback, such as measuring pressure or identifying tissue types.
For instance, some advanced instruments can differentiate between healthy and diseased tissue, helping surgeons make more informed decisions during procedures. Others can monitor surgical conditions and provide alerts, reducing the risk of errors.
The U.S. Food and Drug Administration (FDA) has been actively regulating and approving these advanced medical devices, ensuring they meet strict safety and performance standards.
From a global perspective, the adoption of smart instruments is growing rapidly, especially in developed countries. However, efforts are being made to make these technologies more accessible to developing regions as well.
This classification reflects the future of surgery—where tools are not just passive instruments but active participants in the surgical process. It’s a shift from traditional methods to a more technology-driven approach, improving outcomes and redefining what’s possible in healthcare.
Importance of Proper Instrument Classification
Role in Surgical Efficiency
Let’s face it—surgery is not just about skill; it’s also about speed and coordination. This is where proper classification of surgical instruments plays a huge role in improving surgical efficiency. When instruments are organized and categorized correctly, it allows the surgical team to work seamlessly, without unnecessary delays or confusion.
Imagine being in an operating room where instruments are not properly classified. The surgeon asks for a specific tool, and the assistant struggles to find it. Even a delay of a few seconds can disrupt the flow of the procedure. Now multiply that across a complex surgery, and you can see how critical organization becomes.
Proper classification ensures that:
- Instruments are easily identifiable
- Surgical teams can respond quickly
- Procedures are completed within optimal timeframes
According to the World Health Organization (WHO), efficient surgical practices significantly improve patient outcomes and reduce the risk of complications. Instrument classification is a key part of this efficiency.
It also enhances team coordination. Every member of the surgical team knows exactly where each instrument belongs and how it is used. This creates a smooth workflow, reducing stress and improving overall performance.
Globally, hospitals follow standardized classification systems to maintain consistency. This is particularly important in large healthcare facilities where multiple surgeries are performed simultaneously.
In simple terms, proper classification acts like a well-organized system that keeps everything running smoothly. It ensures that surgeons can focus on the procedure rather than worrying about finding the right tools.
Impact on Patient Safety
While efficiency is important, nothing matters more than patient safety. Proper classification of surgical instruments directly contributes to safer procedures and better outcomes.
One of the biggest risks in surgery is infection, and classification plays a key role in preventing it. Instruments are often grouped based on how they are used and sterilized. This ensures that the correct cleaning protocols are followed for each category.
The Centers for Disease Control and Prevention (CDC) emphasizes that proper handling and categorization of surgical instruments are essential for preventing healthcare-associated infections. This highlights how classification is directly linked to patient safety.
Another important aspect is error prevention. When instruments are clearly classified and organized, the chances of using the wrong tool are significantly reduced. This is especially important in complex surgeries where precision is critical.
Classification also supports inventory management, ensuring that all instruments are accounted for before and after a procedure. This helps prevent situations where tools are accidentally left inside the patient—a rare but serious issue.
From a global perspective, patient safety is a top priority in healthcare systems. Proper classification of instruments is one of the many practices that contribute to achieving this goal.
In essence, classification is not just about organization—it’s about creating a safer environment for patients. It ensures that every tool is used correctly, every time, reducing risks and improving outcomes.
Modern Innovations in Surgical Instrument Classification
AI and Digital Categorization
The future of surgical instrument classification is being shaped by technology, particularly artificial intelligence (AI) and digital systems. These innovations are transforming how instruments are tracked, categorized, and managed in healthcare settings.
AI-powered systems can automatically identify and classify instruments based on their shape, size, and function. This reduces the need for manual sorting and minimizes the risk of human error. For example, advanced imaging systems can recognize instruments in real time and provide data to surgical teams.
Digital tracking systems are also becoming more common. These systems use barcodes or RFID tags to monitor instruments throughout their lifecycle—from sterilization to usage. This ensures complete traceability and improves accountability.
The National Institutes of Health (NIH) highlights the growing role of digital technologies in improving healthcare efficiency and accuracy, including surgical practices.
Globally, these technologies are being adopted in modern hospitals to streamline operations and improve patient care. While still evolving, they represent a significant step forward in surgical innovation.
Global Standardization Systems
As healthcare becomes more interconnected, the need for global standardization in surgical instrument classification is becoming increasingly important. Standardization ensures that instruments are categorized and used consistently across different regions and healthcare systems.
Organizations like the World Health Organization (WHO) and the International Organization for Standardization (ISO) play a key role in developing guidelines and standards for medical devices.
Standardization benefits include:
- Improved communication among healthcare professionals
- Enhanced training and education
- Greater consistency in patient care
It also supports international collaboration, allowing medical teams from different countries to work together effectively.
In simple terms, global standardization creates a common language for surgical instruments, making healthcare more efficient and accessible worldwide.
Conclusion
The classification of surgical instruments is far more than a technical concept—it’s a foundational element of modern healthcare. From improving efficiency in the operating room to enhancing patient safety, proper classification plays a critical role in every aspect of surgical practice.
By organizing instruments based on function, design, usage, and specialization, healthcare professionals can work more effectively and deliver better outcomes. As technology continues to evolve, the future of classification will become even more advanced, integrating AI and global standards.
Understanding this system not only benefits medical professionals but also helps patients appreciate the complexity and precision involved in surgical care.
FAQs
What is the classification of surgical instruments?
It is the systematic grouping of surgical tools based on their function, design, and usage.
Why is classification important in surgery?
It improves efficiency, reduces errors, and enhances patient safety.
What are the main categories of surgical instruments?
Cutting, grasping, clamping, retracting, probing, and suturing instruments.
What is the difference between reusable and disposable instruments?
Reusable instruments are sterilized and used multiple times, while disposable ones are used once and discarded.
How is technology changing surgical instrument classification?
AI and digital systems are automating classification and improving accuracy.
Medical Disclaimer:
“”The information provided in this article is for educational and informational purposes only and is not intended as medical advice. Always consult a qualified healthcare professional for diagnosis, treatment, or medical concerns. The author is not responsible for any outcomes resulting from the use of this information.””