Smart Operating Rooms: How AI & IoT Are Transforming Surgery in 2026
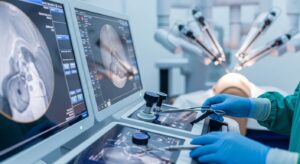
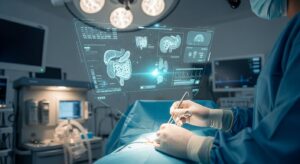
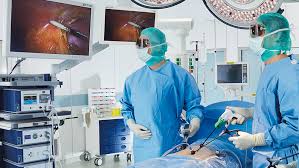
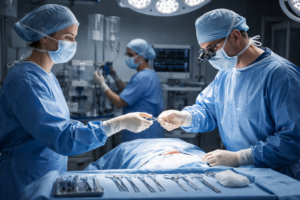
Surgeons utilize AI-powered robotic technology in a futuristic operating room, enhancing precision and patient safety during complex procedures.
The operating room has evolved from a sterile, controlled environment into an intelligent, data-driven ecosystem. As we navigate through 2026, artificial intelligence and the Internet of Things are fundamentally reshaping how surgeries are performed, monitored, and optimized. Smart operating rooms represent the convergence of cutting-edge technology with medical expertise, creating surgical environments that are safer, more efficient, and remarkably precise.
This transformation goes beyond simply introducing new gadgets into the surgical suite. It represents a complete reimagining of how surgical teams work, how decisions are made during procedures, and how patient outcomes are improved through real-time data and intelligent automation.
Understanding Smart Operating Rooms
A smart operating room is a technologically advanced surgical environment where interconnected devices, sensors, and artificial intelligence systems work together seamlessly. These sophisticated spaces integrate robotic surgical platforms, advanced imaging systems, environmental sensors, and real-time analytics to create a comprehensive ecosystem that supports surgical teams throughout every procedure.
Unlike traditional operating rooms that rely primarily on the surgeon’s skill and experience, smart ORs augment human expertise with machine intelligence. Sensors monitor everything from room temperature and humidity to instrument locations and patient vital signs. AI systems analyze this constant stream of data, providing surgical teams with actionable insights that enhance decision-making and improve patient safety.
The modern smart operating room functions as a mission control center where digital displays present live case status, equipment readiness, and potential issues before they become problems. This level of integration and visibility was unimaginable just a few years ago, yet it’s becoming the new standard in hospitals worldwide.
Artificial Intelligence: The Brain Behind Smart Surgery
Artificial intelligence serves as the connective tissue that transforms raw data into meaningful surgical intelligence. Machine learning algorithms and predictive analytics power an entirely new generation of surgical support systems that assist medical teams in ways previously impossible.
Real-Time Decision Support
During surgical procedures, AI systems analyze medical imaging, patient histories, and current vital signs simultaneously. These platforms can identify critical anatomical structures like blood vessels and tumors with remarkable accuracy, reducing the risk of surgical errors. Computer vision technology helps surgeons navigate complex procedures by highlighting important features and providing guidance based on thousands of previous similar cases.
The da Vinci 5 robotic surgery system exemplifies this advancement, offering real-time feedback during operations alongside comprehensive post-operative reports. Surgeons receive performance insights similar to professional athletes reviewing game footage, creating a continuous improvement loop that enhances surgical precision over time.
Predictive Analytics for Surgical Planning
AI doesn’t just assist during surgery—it revolutionizes pre-operative planning. Advanced algorithms analyze patient data to predict optimal surgical approaches, potential complications, and expected procedure durations. This predictive capability allows surgical teams to prepare more thoroughly and allocate resources more efficiently.
Digital twin technology creates virtual replicas of patients and surgical scenarios, enabling surgeons to practice complex procedures before entering the operating room. These simulations incorporate patient-specific anatomy and anticipated challenges, significantly reducing uncertainty when the actual surgery begins.
Automated Documentation and Workflow
Ambient AI systems listen to conversations in the operating room, transcribe key information, and automatically populate electronic health records. This technology frees surgeons and their teams from administrative burdens, allowing them to focus entirely on the procedure at hand. By 2026, these systems have become remarkably context-aware and reliable, seamlessly integrating into surgical workflows without disrupting the team’s concentration.
Internet of Things: Creating Connected Surgical Environments
The Internet of Things brings unprecedented connectivity to operating rooms, linking devices, equipment, and monitoring systems into a unified network. This interconnectedness enables real-time coordination and responsiveness that transforms how surgical procedures are managed.
Environmental Monitoring and Control
IoT sensors continuously track environmental conditions within operating rooms, including temperature, humidity, and air quality. Maintaining optimal conditions is crucial for patient safety and successful outcomes. Smart systems automatically adjust environmental controls when conditions drift outside acceptable parameters, ensuring the surgical field remains sterile and comfortable.
These same sensors monitor equipment sterilization status, alerting staff when instruments require cleaning or when sterile fields may have been compromised. This constant vigilance reduces infection risks and helps maintain the highest safety standards throughout every procedure.
Intelligent Asset Tracking
Hospitals deploy Real-Time Location Systems using Bluetooth beacons, RFID tags, and QR codes to track valuable surgical equipment. These IoT-enabled tracking systems ensure that critical instruments are always available when needed and help prevent costly equipment losses. Surgical teams can locate specific tools instantly rather than wasting precious minutes searching for misplaced items.
Beyond simple location tracking, smart asset management systems monitor equipment performance and predict maintenance needs before failures occur. This predictive maintenance capability minimizes equipment downtime and ensures surgical tools function properly when lives depend on them.
Patient Monitoring Systems
Wearable biosensors and advanced monitoring devices create comprehensive pictures of patient health during surgery. These IoT devices track vital signs continuously, transmitting data wirelessly to centralized systems where AI algorithms analyze patterns and detect anomalies. When a patient’s condition changes unexpectedly, the system immediately alerts the surgical team, enabling rapid intervention.
Some advanced systems even monitor the surgeon’s physical state, tracking fatigue levels and concentration through wearable sensors. This dual monitoring approach ensures both patient and surgeon are in optimal condition throughout lengthy procedures.
Robotic-Assisted Surgery: Precision Meets Intelligence
Robotic surgical systems have evolved dramatically, moving from simple tool control to intelligent surgical assistance powered by AI and advanced imaging. These platforms combine mechanical precision with computational intelligence to expand what’s surgically possible.
Enhanced Surgical Dexterity
Modern robotic systems like the da Vinci platform, Medtronic’s Hugo system, and CMR Surgical’s Versius provide surgeons with enhanced dexterity and motion scaling. Robotic arms execute movements with submillimeter precision while filtering out natural hand tremors. This level of control enables minimally invasive procedures that result in smaller incisions, reduced scarring, and faster patient recovery.
The modular design of newer systems allows hospitals to configure robotic arms around patients based on specific procedural needs. This flexibility makes advanced robotic surgery accessible even in smaller operating rooms where traditional fixed-tower systems wouldn’t fit.
AI-Driven Surgical Guidance
Next-generation robotic platforms integrate artificial intelligence to provide active surgical guidance. These systems analyze real-time video feeds from surgical cameras, identifying anatomical structures and suggesting optimal approaches. Some platforms can even execute certain routine tasks autonomously under surgeon supervision, such as suturing or tissue retraction.
Johnson & Johnson’s MONARCH Platform for Urology incorporates AI-driven simulation capabilities where virtual operating environments help clinical teams set up robotic systems before procedures begin. This preparation reduces setup time and minimizes potential configuration errors.
Surgical Specialization and Expansion
Robotic systems are expanding beyond traditional applications into increasingly specialized areas. Cardiovascular and thoracic robotic surgery allows minimally invasive access to the heart without requiring surgeons to crack the sternum. Orthopedic robots assist with joint replacements, using surgical planning software to optimize implant sizing and alignment with remarkable consistency.
Neurosurgery platforms leverage robotic precision for delicate brain procedures where millimeter-level accuracy is essential. As these technologies mature, they’re enabling surgeries that were previously too risky or technically challenging to attempt.
Data-Driven Surgical Ecosystems
The modern operating room generates massive volumes of data from imaging systems, robotic platforms, monitoring devices, and environmental sensors. Converting this information into actionable intelligence represents one of the most significant advances in surgical care.
Comprehensive Performance Analytics
Post-operative analytics platforms provide surgical teams with detailed performance metrics covering every aspect of a procedure. These systems track case duration, instrument usage, complication rates, and recovery outcomes. Surgeons can review their performance similarly to athletes studying game film, identifying areas for improvement and refining techniques over time.
Hospital administrators use this same data to optimize operating room scheduling, improve resource allocation, and identify training needs. The insights derived from surgical data help healthcare systems operate more efficiently while maintaining exceptional care quality.
Interoperability and Integration
For smart operating rooms to reach their full potential, various technologies must communicate seamlessly. Interoperability between AI scheduling systems, robotic platforms, patient monitoring devices, and hospital information systems eliminates workflow bottlenecks and prevents information silos.
Leading healthcare technology companies prioritize platforms that integrate easily with existing hospital infrastructure. This focus on compatibility ensures that investments in smart OR technology deliver maximum value without requiring complete system overhauls.
Real-Time Communication and Coordination
Digital operating room integration systems synchronize information across surgical teams, anesthesiology, nursing staff, and hospital leadership. Live dashboards display case progress, turnover readiness, staffing constraints, and equipment status. This shared visibility enables rapid response to unexpected situations and keeps everyone coordinated throughout busy surgical schedules.
Advanced communication platforms facilitate patient coordination as well, providing accurate surgery time predictions, reducing waiting periods, and proactively communicating delays or rescheduling needs to patients and families.
Enhancing Patient Safety and Outcomes
Every technological advancement in smart operating rooms ultimately serves one purpose: improving patient safety and surgical outcomes. The combination of AI and IoT creates multiple layers of protection that catch potential issues before they impact patients.
Error Prevention and Quality Control
AI systems help prevent surgical errors by verifying patient identity, confirming correct surgical sites, and ensuring all necessary instruments are available before procedures begin. Computer vision technology can detect when surgical sponges or instruments are inadvertently left inside patients, prompting teams to perform final counts before closing incisions.
Smart checklists integrated into operating room management systems ensure that critical safety protocols are followed consistently. These systems guide teams through pre-operative, intraoperative, and post-operative procedures, reducing the likelihood of missed steps that could compromise patient safety.
Reduced Complications and Recovery Time
Studies show that AI-assisted robotic surgeries achieve approximately 25% reduction in operative time and 30% decrease in intraoperative complications compared to traditional manual methods. Minimally invasive robotic procedures result in smaller incisions, less blood loss, reduced pain, and significantly shorter hospital stays.
Patients benefit from these technological advances through faster recoveries, fewer complications, and better long-term outcomes. The precision enabled by smart OR technologies allows surgeons to preserve more healthy tissue while completely addressing surgical targets.
Continuous Monitoring and Early Intervention
IoT-connected monitoring systems track patient vital signs continuously, detecting subtle changes that might indicate developing complications. AI algorithms identify patterns in this data that human observers might miss, triggering alerts when intervention is needed. This early warning capability enables surgical teams to address issues before they become serious, potentially preventing life-threatening situations.
Post-operative monitoring extends beyond the operating room, with connected devices tracking patient recovery and alerting healthcare providers to concerning trends. This continuity of care ensures patients receive appropriate support throughout their entire surgical journey.
Challenges and Considerations in Smart OR Implementation
While the benefits of smart operating rooms are substantial, hospitals face several challenges when implementing these advanced technologies. Understanding and addressing these obstacles is essential for successful adoption.
Cybersecurity and Data Privacy
The proliferation of connected devices and networked systems creates new cybersecurity vulnerabilities. Hospitals must implement rigorous security protocols to protect sensitive patient data and ensure operating room systems cannot be compromised. Encryption, network segmentation, access controls, and regular security audits are essential components of smart OR cybersecurity strategies.
Medical device manufacturers share responsibility for security, building protections directly into surgical robots, monitoring systems, and other connected equipment. Ongoing security updates and patches must be applied consistently to address newly discovered vulnerabilities.
Training and Adoption
Introducing sophisticated AI and IoT technologies requires comprehensive training for surgical teams, nursing staff, and support personnel. Without proper education, there’s risk of underutilization or procedural errors that could compromise both safety and efficiency. Hospitals must invest in robust training programs that ensure all team members can effectively use new technologies.
Resistance to change represents another adoption challenge. Some medical professionals may be skeptical of AI-driven systems or concerned about technology replacing human judgment. Successful implementation requires demonstrating how these tools augment rather than replace medical expertise, empowering clinicians to provide better patient care.
Cost and Resource Allocation
Smart operating room technologies represent significant financial investments. Robotic surgical systems, AI platforms, and IoT infrastructure require substantial upfront capital and ongoing maintenance expenses. Hospitals must carefully evaluate return on investment, considering factors like improved surgical outcomes, increased efficiency, reduced complications, and enhanced patient satisfaction.
Smaller healthcare facilities may struggle to afford cutting-edge technologies that larger academic medical centers can deploy readily. This disparity raises concerns about equitable access to advanced surgical care across different patient populations and geographic regions.
Regulatory Compliance
Medical device regulations vary across countries and regions, impacting how quickly new technologies can be deployed. Stringent approval processes from regulatory bodies like the FDA in North America and EMA in Europe significantly affect market entry and growth. While these regulations protect patient safety, they can slow the introduction of beneficial innovations.
Hospitals must ensure that all smart OR technologies comply with relevant regulations and that proper documentation and reporting procedures are followed. Maintaining compliance requires dedicated resources and attention as technologies evolve and regulations change.
The Future of Smart Operating Rooms
Looking beyond 2026, the trajectory of smart operating room technology points toward even greater integration, autonomy, and personalization. Several emerging trends will likely shape the next generation of surgical care.
Increased Autonomy and Semi-Autonomous Surgery
As AI systems become more sophisticated and reliable, we’ll see gradual movement toward semi-autonomous surgical procedures. These systems won’t replace surgeons but will handle increasingly complex routine tasks under expert supervision. Computer vision models are already demonstrating autonomous suturing capabilities in research settings, suggesting that certain surgical sub-tasks could eventually be performed with minimal human intervention.
The goal is not complete automation but rather freeing surgeons to focus on critical decision-making and complex aspects of procedures while AI handles predictable, repetitive tasks with consistent precision.
Extended Reality Integration
Augmented reality and virtual reality technologies will become more deeply integrated into smart operating rooms. Surgeons may use AR headsets that overlay patient-specific anatomical information directly onto their field of view during procedures. VR platforms will enable more sophisticated pre-operative planning and remote surgical training, allowing experts to share knowledge globally.
These extended reality interfaces will integrate seamlessly with robotic systems and AI platforms, creating immersive surgical environments that blend physical and digital realities.
Global Collaboration and Knowledge Sharing
Connected operating rooms will facilitate unprecedented global collaboration among surgical teams. Experts in different countries could virtually participate in complex procedures, providing guidance and consultation in real-time. Data-driven learning loops will allow surgical platforms to incorporate insights from procedures performed worldwide, continuously improving performance based on collective global experience.
This knowledge sharing could help reduce disparities in surgical care quality between different regions and healthcare systems, democratizing access to cutting-edge surgical expertise.
Personalized Surgical Approaches
As AI systems analyze larger datasets encompassing thousands of patient outcomes, they’ll provide increasingly personalized surgical recommendations. These platforms will consider individual patient characteristics, genetic factors, and predicted responses to different surgical approaches, enabling truly customized treatment plans.
Precision surgery will evolve beyond current techniques, with AI suggesting optimal incision locations, tissue handling strategies, and post-operative care protocols tailored to each patient’s unique physiology and circumstances.
FAQs
What makes an operating room “smart” in 2026?
Smart operating rooms in 2026 integrate AI-powered systems, IoT-connected devices, robotic surgical platforms, and advanced analytics to create intelligent surgical environments. These spaces feature interconnected sensors monitoring everything from environmental conditions to patient vital signs, AI systems providing real-time decision support, automated documentation tools, and comprehensive data analytics platforms that optimize surgical workflows and improve outcomes. The “smart” designation refers to the room’s ability to actively support surgical teams through technology rather than simply providing a sterile space for procedures.
How does AI actually help surgeons during operations?
AI assists surgeons in multiple ways during operations. Computer vision systems analyze surgical camera feeds in real-time, identifying critical anatomical structures like blood vessels and organs while alerting surgeons to potential issues. AI platforms provide decision support by analyzing patient data and suggesting optimal approaches based on similar previous cases. Predictive algorithms anticipate complications before they occur, giving teams time to prepare appropriate interventions. Some systems also provide performance feedback during procedures, helping maintain optimal surgical technique throughout lengthy operations. Importantly, AI doesn’t make surgical decisions—it augments the surgeon’s expertise with data-driven insights.
Are robotic surgeries safer than traditional manual procedures?
Research demonstrates that AI-assisted robotic surgeries generally achieve better outcomes than traditional manual approaches. Studies show approximately 25% reduction in operative time and 30% decrease in intraoperative complications with robotic systems. These platforms provide enhanced precision, tremor filtration, and superior visualization that enable minimally invasive procedures resulting in smaller incisions, less bleeding, reduced pain, and faster patient recovery. However, safety depends significantly on proper training and appropriate patient selection. Robotic surgery works best when experienced surgical teams use the technology for suitable procedures rather than attempting to replace all manual surgery.
What happens to patient data collected by smart OR systems?
Patient data collected by smart operating room systems is protected under strict privacy regulations and security protocols. Information flows through encrypted channels and is stored in secure, compliant systems that meet healthcare data protection standards. Access is restricted to authorized healthcare providers involved in patient care, with detailed audit trails tracking who views data and when. Advanced cybersecurity measures including network segmentation, multi-factor authentication, and regular security updates protect against unauthorized access. Many systems also anonymize data used for research and quality improvement purposes, separating personal identifiers from clinical information. Patients typically provide consent for data collection and use as part of surgical consent processes.
How long before smart operating rooms become standard worldwide?
Adoption timelines vary significantly based on geographic location, healthcare system resources, and hospital size. Major academic medical centers and large hospital systems in developed countries are already implementing smart OR technologies extensively, with many facilities having comprehensive systems in place by 2026. Mid-sized hospitals are following rapidly, particularly as modular, more affordable solutions become available. Smaller healthcare facilities and hospitals in developing regions face longer adoption timelines due to cost constraints and infrastructure limitations. However, the trend is clearly toward widespread adoption—experts predict that within the next five to ten years, smart operating room technologies will become standard expectations rather than cutting-edge innovations, similar to how minimally invasive surgery evolved from specialty practice to routine care.
Conclusion
Smart operating rooms represent one of the most significant advances in modern healthcare, fundamentally transforming how surgeries are performed and managed. The integration of artificial intelligence and Internet of Things technologies creates surgical environments that are safer, more efficient, and remarkably precise. These intelligent ecosystems augment human expertise with machine intelligence, enabling surgical teams to achieve outcomes that were previously impossible.
The journey from traditional operating rooms to smart surgical suites reflects broader trends in healthcare toward data-driven decision-making, personalized medicine, and technology-enabled care. As we progress through 2026 and beyond, these technologies will continue evolving, bringing increased autonomy, better integration, and more personalized surgical approaches.
Challenges remain—cybersecurity concerns, training requirements, cost considerations, and regulatory complexities must all be addressed thoughtfully. However, the benefits to patient safety, surgical outcomes, and healthcare efficiency make continued investment in smart operating room technologies not just worthwhile but essential.
For patients, these advances mean safer surgeries, faster recoveries, and better long-term outcomes. For surgical teams, smart ORs provide powerful tools that enhance capabilities and reduce burdens. For healthcare systems, these technologies offer pathways to improved efficiency and quality while managing growing demand for surgical services.
The operating room of 2026 is smarter, more connected, and more capable than ever before. As artificial intelligence and Internet of Things technologies continue advancing, the future of surgery looks increasingly bright, promising better care for patients worldwide.